
Effective policies and strategies to impact this goal include:
Children are born healthy to healthy parents, and pregnancy experiences and birth outcomes are equitable.

WHY IS HEALTHY AND EQUITABLE BIRTHS AN IMPORTANT PRENATAL-TO-3 GOAL?
Setbacks and trauma that children and families experience due to often preventable pregnancy and birth complications can have lifelong consequences for children’s health and wellbeing. Many babies in the US are born thriving, but each child who is not may need substantial resources and care not just to survive infancy but to meet the challenges beyond.1 A child born prematurely arrives before the 37th week of pregnancy, a time during which the rapidly developing brain and other organs still benefit dramatically from the unique advantages of the intrauterine environment.2 Premature birth increases the likelihood of low birthweight (less than 2,500 grams), which predisposes children to breathing and feeding difficulties, vision and hearing problems, developmental delays, and learning disabilities, among other short- and long-term complications.3
Adverse birth outcomes disproportionately affect Black families. Compared to White and Hispanic infants and mothers, Black infants are more likely to be born low birthweight,4 and Black mothers are more than twice as likely to die in childbirth5 or experience severe maternal morbidity6 —regardless of education level or socioeconomic status.7 Pregnant people need adequate health care over the life course to ensure a healthy pregnancy, and disparities can be a reflection of exposure to adversity across the lifespan.8 Supporting people who may become pregnant throughout the life course increases the likelihood of healthy pregnancies, fewer birth complications, and healthier newborns.9
MATERNAL MORTALITY RATE
The number per 100,000 women who were pregnant who died while pregnant or within 42 days of pregnancy, “from any cause related to or aggravated by the pregnancy or its management, but not from accidental or incidental causes.”
US Average: 23.8 deaths per 100,000
White, non-Hispanic: 19.1 deaths per 100,000
Hispanic: 18.2 deaths per 100,000
Black, non-Hispanic: 55.3 deaths per 100,000
Definition Source: Centers for Disease Control and Prevention. (2019). Pregnancy-related deaths. https://www.cdc.gov/reproductivehealth/maternalinfanthealth/pregnancy-relatedmortality.htm
Data Source: Hoyert, D. L. (2022). Maternal mortality rates in the United States, 2020. NCHS Health E-Stats. DOI: https://dx.doi.org/10.15620/cdc:113967 .
Our comprehensive reviews of rigorous research show that solutions currently pursued by some states, including Medicaid expansion and policies boosting families’ financial resources, can be effective in promoting healthy and equitable pregnancy and birth experiences.
HOW ARE STATES CURRENTLY MEETING THIS PRENATAL-TO-3 GOAL?
Two outcome measures illustrate the health of babies at birth, which is often also an indicator of maternal health during the perinatal period: (1) preterm births and (2) infant mortality. Birth outcomes vary considerably across states, as well as by race and ethnicity. Maternal mortality and morbidity are also important indicators of healthy and equitable births, but the sample sizes of the data are too small to measure these outcomes at the state level. Racial and ethnic disparities in these outcomes reveal long-standing patterns of racism and policy choices within states that discriminate against families of color. Eliminating these disparities must be a goal for all states.
Both outcome measures were calculated intentionally in the negative direction to demonstrate where states have room for improvement and to help states prioritize the prenatal-to-3 policy goals. Out of 51 states, the state lagging furthest behind ranks 51st, and the leading state ranks first. The median state indicates that half of states have outcomes that measure better than that state, whereas half of states have outcomes that are worse. Importantly, the “leading” state on a given outcome does not necessarily indicate a target for all other states to strive toward; even in the states with the best outcomes, many children and families are struggling.
OUTCOME MEASURE: PRETERM BIRTHS
% of babies born prior to preterm (<37 weeks)
Median state value: 9.9%
Preterm delivery is associated with subsequent negative health and developmental outcomes for children, and it is often an indication of poor maternal health during the pregnancy. Approximately 1 out of every 10 babies is born before the 37th week of gestation in the US, but that number varies considerably across states; for example, 14.2% of babies are born preterm in Mississippi, compared to 7.6% of babies in Vermont. The percentage of Black infants who are born preterm is approximately 50% higher than White or Hispanic infants.
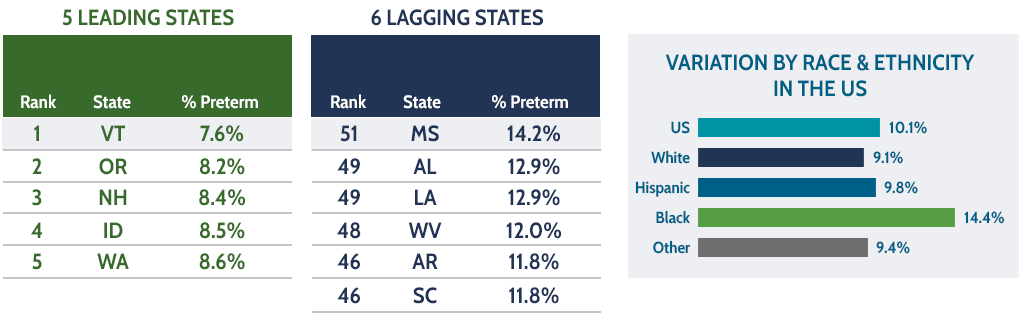
Source: Vital Statistics from CDC WONDER 2020 Natality.
OUTCOME MEASURE: INFANT MORTALITY RATE
# of infant deaths per 1,000 births
Median state value: 5.4
In the five lagging states, more than twice as many children die in their first year of life as in the seven leading states. Black families are disproportionately likely to experience this traumatic loss: In 2020, from the most recent disaggregated data available, the number of Black infants who die in the first year of life was more than double the number of White or Hispanic infants.
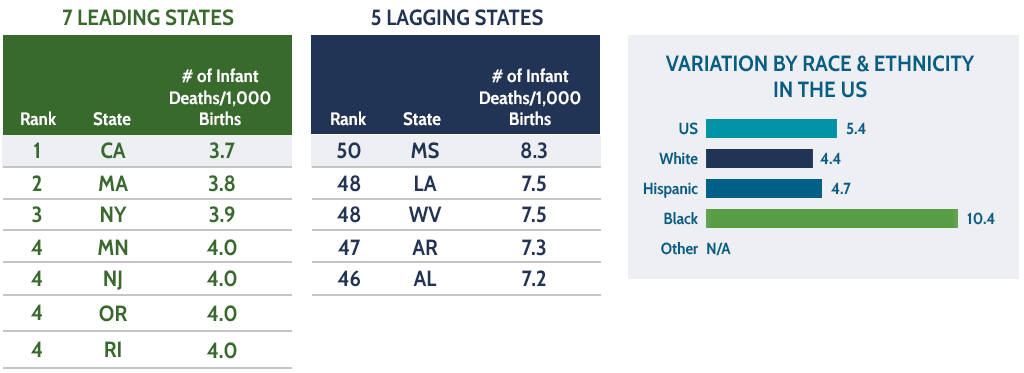

Sources: State estimates: CDC National Center for Health Statistics (NCHS), States of the States: Infant Mortality Rates by State.
National estimates: National Vital Statistics Reports, Infant mortality in the United States, 2020: Data from the period linked birth/infant death file.
Note: One state (Vermont) had unreliable data due to a small sample size. Rankings are calculated out of 50 states instead of 51 for this measure.
For additional information regarding calculation details, data quality, and source data please refer to Methods and Sources.
For more information on outcomes by goal, including by race and ethnicity and state, see the 2022 Prenatal-to-3 State Policy Roadmap section on outcomes across the US.
WHAT ARE THE MOST EFFECTIVE POLICIES AND STRATEGIES TO IMPACT HEALTHY AND EQUITABLE BIRTHS?
Based on comprehensive reviews of the most rigorous evidence available, the Prenatal-to-3 Policy Impact Center identified 11 effective solutions that foster the nurturing environments infants and toddlers need. For each of the five policies, the evidence points to a specific policy lever that states can implement to impact outcomes. For the six strategies, the evidence clearly links the strategy to PN-3 outcomes, but the current evidence base does not provide clear guidance on how states should implement each strategy to positively impact outcomes. Three policies have demonstrated effectiveness at improving families’ access to needed services.
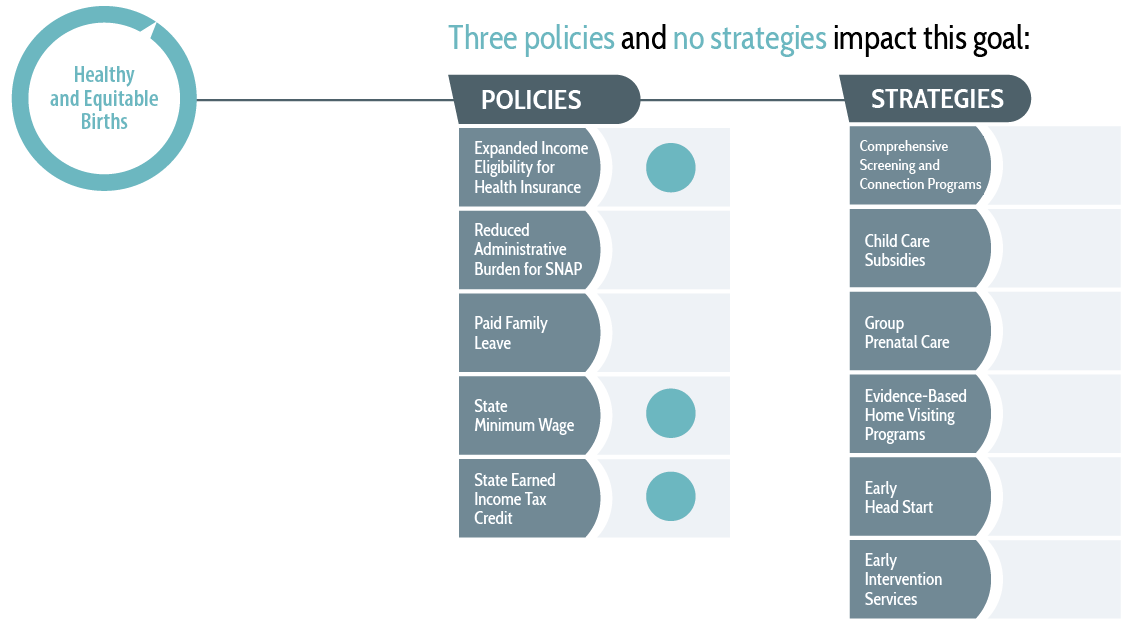
For more information on the impact of state-level policies and strategies in the prenatal-to-3 period, search the Prenatal-to-3 Policy Clearinghouse for an ongoing inventory of rigorous evidence reviews. To learn more about the impact of effective policies and strategies on the eight prenatal-to-3 policy goals, see the Prenatal-to-3 State Policy Roadmap.
WHAT OTHER SOLUTIONS ARE STATES PURSUING THAT CAN HELP BUILD THE EVIDENCE BASE?
Beyond the policies and strategies proven effective by the current research, states also are pursuing other approaches that hold promise for improving healthy and equitable births; these approaches have not yet accumulated enough rigorous research to enable drawing conclusions on their effectiveness, or the Prenatal-to-3 Policy Impact Center has not yet conducted a comprehensive evidence review for the approach. Other solutions states are pursuing that can help build the evidence base on healthy and equitable births include, but are not limited to:
- Perinatal Quality Collaboratives and Maternal Mortality Review Committees (PQCs and MMRCs), which are statewide, multidisciplinary networks that promote evidence-based clinical practices by bringing key stakeholders together, producing issue briefs and strategic plans, and holding symposia and other events;10
- Participation in the Alliance for Innovation on Maternal Health (AIM), an alliance working to bring health improvement efforts for pregnant people at the national, state, and hospital level into alignment by providing hospitals with toolkits and bundles of medical information;11
- Implicit-bias training, which teaches medical professionals how to recognize and understand racial and cultural differences and biases, as well as how to interact with patients in a way that is sensitive to these differences and accommodates patients’ diverse needs;12
- Funding doula services, such as through Medicaid to increase access to physical, emotional, and educational support for pregnant people;13 and
- Extending Medicaid coverage to 12 months postpartum: States can extend Medicaid coverage beyond the current federal minimum of 60 days postpartum. The increase of the eligibility for health insurance should improve health insurance coverage and maternal health outcomes during the postpartum period.14
SOURCES
- National Institutes of Child Health and Human Development. (2012). The long-lasting effects of preterm birth. US Department of Health and Human Services (HHS). https://www.nichd.nih.gov/newsroom/resources/spotlight/012612-effects-preterm-birth
- Institute of Medicine (US) Committee on Understanding Premature Birth and Assuring Healthy Outcomes (2007). Preterm birth: Causes, consequences, and prevention. Behrman, R. E., & Butler, A. S. (Eds.). Washington (DC): National Academies Press (US). https://www.ncbi.nlm.nih.gov/books/NBK11382/
- National Institutes of Child Health and Human Development. (2012). The long-lasting effects of preterm birth. US Department of Health and Human Services. https://www.nichd.nih.gov/newsroom/resources/spotlight/012612-effects-preterm-birth
- Martin, J. A., Hamilton, B. E., Osterman, M. J. K., Driscoll, A. K. (2019, November 27). Births: Final data for 2018. National Vital Statistics Reports, 68(13). 1-47. Hyattsville, MD: National Center for Health Statistics. https://www.cdc.gov/nchs/data/nvsr/nvsr68/nvsr68_13-508.pdf
- Hoyert, D. L., & Miniño, A. M. (2020). Maternal mortality in the United States: Changes in coding, publication, and data release, 2018. National Vital Statistics Reports, 69(2). 1-18. Hyattsville, MD: National Center for Health Statistics. https://www.cdc.gov/nchs/data/nvsr/nvsr69/nvsr69-02-508.pdf
- Creanga, A. A., Bateman, B. T., Kuklina, E. V., & Callaghan, W. M. (2014). Racial and ethnic disparities in severe maternal morbidity: A multistate analysis, 2008-2010. American Journal of Obstetrics and Gynecology, 210(5), 435.e1–435.e8. https://doi.org/10.1016/j. ajog.2013.11.039
- Novoa, C., & Taylor, J. (2018, February 1). Exploring African Americans’ high maternal and infant death rates. Center for American Progress. https://www.americanprogress.org/ issues/early-childhood/reports/2018/02/01/445576/exploring-african-americans-high-maternal-infant-death-rates/
- Lu, M. C., Kotelchuck, M., Hogan, V., Jones, L., Wright, K., & Halfon, N. (2010). Closing the Black-White gap in birth outcomes: a life-course approach. Ethnicity & Disease, 20(1 Suppl 2), S2–62-76.
- Fine, A., & Kotelchuck, M. (2010, November). Rethinking MCH: The life course model as an organizing framework: Concept paper. HHS, Health Resources and Services Administration, Maternal and Child Health Bureau. https://www.hrsa.gov/sites/default/files/ourstories/mchb75th/images/rethinkingmch.pdf
- Hayes, T. O., & McNeil, C. (2019, September 9). Maternal mortality in the United States. American Action Forum. https://www.americanactionforum.org/insight/maternal-mortality-in-the-united-states/
- Mahoney, J. (2018). The alliance for innovation in maternal health care: A way forward. Clinical Obstetrics and Gynecology, 61(2), 400-410. doi: 10.1097/GRF.0000000000000363
- California Maternal Quality Care Collaborative. (2019). Birth equity. https://www.cmqcc.org/qi-initiatives/birth-equity
- Kozhimannil, K. B., Hardeman, R. R., Alarid‐Escudero, F., Vogelsang, C. A., Blauer‐Peterson, C., & Howell, E. A. (2016). Modeling the cost-effectiveness of doula care associated with reductions in preterm birth and cesarean delivery. Birth, 43(1), 20–27. https://doi.org/10.1111/birt.12218
- Kaiser Family Foundation (As of 2021, September 16). Medicaid postpartum coverage extension tracker. https://www.kff.org/medicaid/issue-brief/medicaid-postpartum-coverage-extension-tracker/
